Off the Beaten Path: Private Capital Transforming the Health of Rural America

Off the Beaten Path: Private Capital Transforming the Health of Rural America

Off the Beaten Path: Private Capital Transforming the Health of Rural America

More than 60 million people live in the rural United States,1 and we believe many are facing a healthcare access crisis. Hospital closures, clinician shortages, and geographic isolation have created healthcare deserts, leading to delayed care, worsening conditions, and higher mortality rates. Encouragingly, innovative private companies are emerging with tailored solutions—from urgent-care clinics to advanced telehealth—designed to deliver quality care efficiently to these underserved populations. We see potential opportunities to invest in companies with intrinsic competitive advantages, targeting both positive financial returns and improved healthcare outcomes.
Constraints on Care
Millions of Americans live in areas with a deficit of primary-care practitioners and mental-health practitioners. These longstanding access barriers are compounded by recent reductions in public funding, with millions of vulnerable individuals, including many in rural areas, projected to lose Medicaid coverage as pandemic-era provisions unwind.
- Hospital Closures: Since 2005, 195 rural hospitals have closed or converted, eliminating inpatient services, and 700 more—roughly one-third of the remaining total—are at high risk of closure.2 We believe these closures are driven by declining populations, high rates of uncompensated care, and insufficient reimbursement. The loss of a local hospital forces residents to travel long distances for emergency and inpatient care, which we believe delays essential treatment. Private equity can intervene by providing capital for operational restructuring, technology upgrades, or by facilitating conversions to more sustainable models like critical access hospitals or specialized outpatient centers, thereby preserving essential services.
- Retreat of Retail Clinics: Even large retailers, once seen as alleviators of access problems, are scaling back or shuttering rural clinics.3 Their withdrawal underscores the difficulty of maintaining profitability and operational efficiency in sparsely populated areas, where low patient volumes and high operational costs challenge long-term viability. This creates an opportunity for private equity-backed specialized providers to step in and support focused, efficient, and community-integrated models, leveraging operational expertise to achieve profitability where larger, less agile players have struggled.
- Clinician Shortages: Recruiting and retaining medical professionals in rural areas remains a significant hurdle. Nearly one-third of rural hospitals report insufficient staffing leading to the closure of vital services (e.g. obstetrics, mental healthcare, and surgical units).4 Clinicians are often deterred by professional isolation, higher patient volumes, and a lack of amenities, professional opportunities, or financial incentives that attract talent to urban centers. Private equity firms can support companies in developing innovative talent solutions, such as using nurse practitioners and leveraging telehealth, with the goal of reducing clinician burden in underserved areas.
- 93
- Million AmericansLive in areas with a deficit of primary-care practitioners.
- 137
- Million AmericansLive in areas facing a shortage of mental-health practitioners.
- 700
- Hospitals at riskAbout one-third of the total remaining in the US are at risk of closure.
Health workforce shortage areas source: Health Resources and Services Administration. As of January 26, 2026. Hospitals at risk source: Rural Hospitals at Risk of Closing, Center for Healthcare Quality & Payment Reform. As of January 2026.
The Cost of Inaction and the Opportunity for Innovation
The consequences of the healthcare access crisis are severe and costly. Rural residents often rely on emergency rooms for non-emergent needs, a practice that is both inefficient and expensive; ER visits can be 10 times more costly than urgent-care alternatives.5 This strains overburdened emergency departments, leading to longer wait times and compromised care for true emergencies. Delays in securing primary-care appointments allow manageable conditions to escalate, increasing treatment complexity and cost. Geographic isolation further exacerbates these issues, as long travel distances become a significant barrier for vulnerable populations lacking reliable transportation, resulting in missed appointments and worse health outcomes.
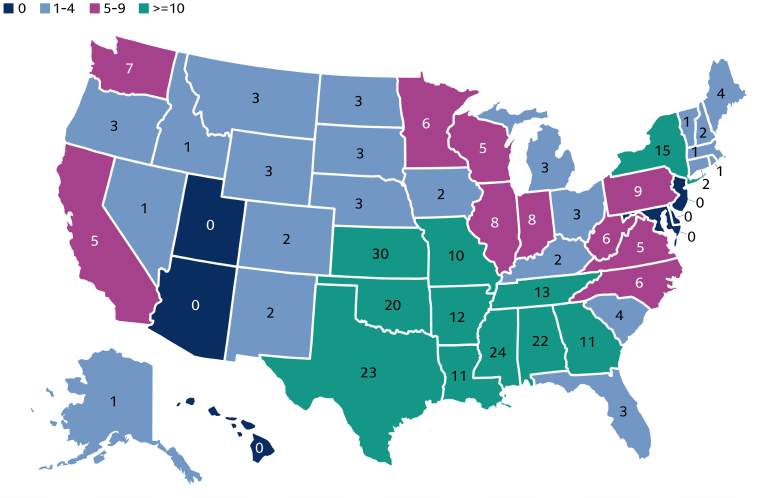
Source: Center for Healthcare Quality & Payment Reform, Goldman Sachs Asset Management. As of January 2026.
A lack of access translates to lower rates of preventative care, such as cancer screenings and vaccinations.6 The result is higher rates of avoidable diseases, late-stage diagnoses, and ultimately, increased mortality from conditions that could have been effectively managed with early intervention. This cycle of delayed and forgone care not only impacts individual health but also places immense strain on the broader healthcare system and local economies.
Innovative Solutions and Potential Investment Opportunities
These challenges make the rural healthcare landscape ripe for investment in innovative solutions. We see a new generation of healthcare providers demonstrating that quality care can be delivered effectively and profitably in rural settings.
Healthcare Company X is a provider of urgent care services to rural and underserved communities. It operates a number of clinics across the South-Centras US, most of which are certified Rural Health Clinics (RHCs). It also provides workers’ compensation and employee service needs, such as physical exams and drug tests, and operates post-acute and behavioral health businesses. This company is able to employ Advanced Practice Providers (primarily nurse practitioners and physician's assistants) for the majority of its patient care needs, while having supervising clinicians available remotely.
- Developing scalable solutions: Urgent-care clinics are proving effective by offering accessible, affordable services—from laboratory tests and X-rays to treatment for common conditions—alleviating pressure on emergency rooms and providing a crucial local access point. Their decentralized model allows for rapid deployment and adaptation to local needs, making them a cornerstone of rural healthcare infrastructure. Telehealth, too, is transforming access, connecting patients with specialists regardless of distance, overcoming geographic barriers, and expanding the reach of limited medical personnel. Beyond basic consultations, we observe advanced telehealth platforms enabling remote monitoring for chronic conditions, virtual mental health services, and even specialized diagnostics, creating efficiencies and improving patient outcomes that were previously unattainable in remote areas. We believe private equity investment is critical for funding the expansion of these models, enabling companies to build out new clinics, invest in advanced telehealth infrastructure, and develop sophisticated operational frameworks necessary for rapid, sustainable growth across diverse rural geographies.
- Addressing staff shortages: Healthcare Company X operates an urgent care model that leverages nurse practitioners. Expanding the role of nurse practitioners is a proven strategy to address physician shortages. NPs are trained to diagnose, treat, and prescribe, as well as manage patient care, and research shows that they can manage up to 90% of primary-care needs.7 In many rural markets, this expanded scope has effectively created a clinical moat: NPs are more likely than physicians to practice in underserved areas, and evidence consistently shows that patient outcomes under NP‑led care are comparable to physician‑led models across primary care and chronic‑disease management.8 Empowering NPs with the right tools, supervision, and full practice authority has led to improved access as well as physician job satisfaction and retention, reduced wait times, and better health outcomes in many rural regions. Private equity can support companies in implementing technology solutions that optimize NP workflows, provide remote physician supervision, and facilitate continuous education, further enhancing their effectiveness and reach in underserved communities. NPs are already helping to fill care gaps, and we believe their numbers are expected to grow significantly, around 40–46% from 2024 to 2034.9
- Improving return potential through RHC designation: State and federal programs, such as the RHC designation, which receives cost-based reimbursement for providing outpatient primary care and preventive services to Medicare and Medicaid patients, are also making it more economically attractive for companies (including our example) to operate in rural areas. Since its inception, the RHC program has grown to more than 5,700 clinics, reflecting ongoing demand for accessible rural healthcare.10 These clinics are a critical component of rural healthcare infrastructure, ensuring even the most vulnerable residents have access to essential services.
The Advantage of an Outcome-Oriented Approach
We believe an outcome-oriented approach in rural healthcare provides a strategic lens for identifying superior financial return opportunities and building resilient portfolios. By rigorously evaluating companies on quality of care, patient experience, and community trust, private equity investors can actively identify ventures with intrinsic competitive advantages and deploy capital to drive operational improvements. These businesses achieve higher patient retention, favorable reimbursement, and greater market share.
In our view, investing in solutions that genuinely improve health outcomes aligns with robust financial performance, transforming a critical social challenge into a compelling and sustainable investment thesis offering both significant capital appreciation and measurable positive impact.
The challenges facing rural healthcare in America are undeniable, but so too is the immense opportunity for strategic investment. By backing innovative privately-owned companies with tailored business models and a commitment to quality, private equity can provide the flexible capital, strategic oversight, and operational expertise crucial for scaling these solutions. In our view, the convergence of unmet demand, technological advancements, and a clear path to sustainable profitability makes rural healthcare a compelling frontier for those seeking both positive financial returns and improved healthcare outcomes.
1 National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Population Health and Public Health Practice; Roundtable on Population Health Improvement; Nicholson A, editor. Population Health in Rural America in 2020: Proceedings of a Workshop. Washington (DC): National Academies Press (US); 2021 Apr 22. 2, Rural America in Context. Available from: https://www.ncbi.nlm.nih.gov/books/NBK575082/
2 The Cecil G. Sheps Center for Health Services Research at The University of North Carolina at Chapel Hill, as of January 26, 2026.
3 HealthLeaders Media. “When the Disruptors are Disrupted: Why Retailers are Tapping Out,” as of July 17, 2024.
4 Center for Healthcare Quality & Payment Reform. “Rural Hospitals at Risk of Closing,” as of July 2024.
5 Allen L, Cummings JR, Hockenberry JM. The impact of urgent care centers on nonemergent emergency department visits. Health Serv Res. 2021 Aug;56(4):721-730. doi: 10.1111/1475-6773.13631. Epub 2021 Feb 8. PMID: 33559261; PMCID: PMC8313962.
6 Loftus J, Allen EM, Call KT, Everson-Rose SA. Rural-Urban Differences in Access to Preventive Health Care Among Publicly Insured Minnesotans. J Rural Health. 2018 Feb;34 Suppl 1(Suppl 1):s48-s55. doi: 10.1111/jrh.12235. Epub 2017 Mar 14. PMID: 28295584; PMCID: PMC6069955.
7 American Association of Nurse Practitioners, “ Nurse Practitioners in Primary Care,” as of October 2025.
8 Htay M, Whitehead D. The effectiveness of the role of advanced nurse practitioners compared to physician-led or usual care: A systematic review. Int J Nurs Stud Adv. 2021 Jun 17;3:100034. doi: 10.1016/j.ijnsa.2021.100034. PMID: 38746729; PMCID: PMC11080477.
9 NurseJournal. “Nurse Practitioners Third Fastest-Growing Occupation in the U.S.” as of September 9, 2025.
10 Rural Health Information Hub, “Rural Health Clinics (RHCs),” as of October 2025.
